What Every Nurse Wants You to Know: 5 Ways to Engage
200,000 nurses graduating each year and yet only 45% are engaged in their work
In the United States, we are training more nurses than ever, graduating just over 200,000 new nurses in 20141. Yet, the reality is that 23 percent of nurse turnover occurs in the first year2. Often, we lose these nurses not just to a new practice environment but to the profession itself. This cost in individual and societal dollars produces a financial burden that impacts the nurse, our healthcare systems, and our communities. While this “churn” invites more students into the profession, achieving the goal of providing healthcare excellence, which requires nursing engagement, becomes more elusive. Recently, we partnered with PRC (Professional Research Consultants) to study nurse engagement. This blog highlights some of our findings and provides pragmatic strategies leaders can adopt. Download a copy of the national nursing study.
While nurses comprise the largest segment of the acute healthcare workforce, only 45 percent feel fully engaged and only 57 percent feel a sense of ownership in their organizations3. Given that we continue to find ourselves in the midst of a shortage of bedside nurses4, we have not just an opportunity but an imperative to provide support to an environment in which nurses feel engaged as owners in their places of work.
What are the ways we can intervene in this destructive cycle of training, orienting, disillusionment, and drop out to provide an environment that serves our patients and our workforce well? How can we make accessible to every nurse a workplace that brings the best of each one in order to carry out that purpose for which they became nurses in the first place?
In its study of 37 nationally representative hospitals, the PRC study revealed three key drivers predicting nursing engagement: Nurse autonomy, RN to RN teamwork and collaboration, and leader access and responsiveness.3 Here are five ways we can help nurses own their autonomy, foster teamwork, and collaboration, and have access to and responsiveness from leaders.
1. Be Curious
Be curious in every single person; be interested in what they uniquely bring to our organizations. Look them in the eye and get to know them; as a person, with life interests and dreams outside the workplace, really see them. Discover their talents and help them develop their gifts.
In our busyness, with our obligations and systems and processes, we sometimes ignore or forget that while our healthcare staff is serving our patients, our mission is to serve our staff. We as leaders have one job and that job is to provide an environment that makes the miraculous possible, whether those miracles are patient cures or healing or comfort or employee growth. We facilitate growth in those who make the patient miracles happen and that growth comes not just in the form of technical and clinical skills but also develop as human beings so that these nurses approach patients from stances of empathy, integrity, and compassion.
Ways to be curious. Use every informal opportunity to learn about your workforce—in the cafeteria line, during forums, through email responses, during your organization’s celebrations. Develop formal ways of getting to know staff; one of the best is through purposeful rounding, designed to spotlight what is working well and praise those who are doing it. This rounding gives us a window into that staff member and his or her perspectives on our organization and their peers. Ask questions, and remember to share things about yourself too.
2. Diminish Unnecessary Stress
Do you ever stop to ask yourself how much we expect from every single person who works in our organizations? Every day, every night, every shift we ask every person to show up as their best selves regardless of the situations happening within those shifts or in their personal lives. Our wisdom allows us to empathize and support our nurses so they can deliver more than we might have believed possible. Yet, we know that leaders are three times more engaged than the teams they lead.5 This concept compels us to take the time to understand the perspective of our nurses by making a personal connection with each one and learning about them as people.
We must support our staff versus adding to the stress caused by the very nature of their jobs. Despite our Western conviction that stress is a motivator, eustress (healthy stress) exists largely in physical situations—building bone and developing muscle. Psychological stress is largely detrimental in decision-making, critical thinking, and operating from our own highest center. We only dupe ourselves when we believe that working from a place of intense stress is beneficial. It is incumbent upon us as leaders to foster an environment that enables nurses to function in a state of well-being so that when stressful situations arise, they are able to respond appropriately.
Ways to diminish unnecessary stress. Recognize what is truly important; focus yourself and help focus your staff on these small number of things. They cannot be our healthcare heroes every day if we don’t care for them; their jobs are too big, too ongoingly stressful, too critical. Get out of the way and let them do what they do best. Allow the people closest to the decision point to make critical decisions, whether by developing staff as subject matter experts or by accessing governance councils or problem-focused teams. Learn from them; pay attention when you ask for input, and let them know how you implemented their input.
3. Provide Real Avenues for Ownership
We’ve mentioned governance councils and problem-focused teams above; provide real ways every nurse can be an “owner” in the sense that he or she practices to the full extent of his or her scope of clinical expertise. These people are the source of knowledge in delivering nursing care; we must allow them to teach how to implement best practice care.
What sources does your organization have for learning about the latest research in nursing care? Staff members have access to the best in practice, whether through mentors, research, or continued education. As leaders, you have the ultimate responsibility to foster not only a learning environment but an environment that allows staff to implement that learning.
Ways to provide real avenues for ownership. Provide informal and formal ways to exchange information and then, listen. Listen to understand versus listening to act immediately. Let them tell you how they can own not just their practice but their part in your organization. Understand ways nurses want to contribute and then clear paths to make those contributions possible. In addition, reward clinical progress, whether through clinical ladders for advancement, mentorships or preceptorships that allow nurses to develop nurses with less expertise, or opportunities for research and developing solutions to real nursing problems.
4. Celebrate
Celebrate not just the big victories (and certainly do celebrate those)—the TJC surveys, the accreditations, the new services lines and areas of focus—but also the small wins. Celebrate the Star of the shift, the person who has been recognized by a patient, the unsung hero very few knew went above and beyond to deliver an outcome.
Many times, leaders fall into one of two camps: we simply neglect celebration of the daily acts altogether or we celebrate in superficial ways that miss the mark. Either of these approaches can feel inauthentic and leave employees feeling unappreciated or ignored.
Ways to celebrate. Ask staff what feels right to them and then be sure and follow through with individualized and meaningful approaches. Change it up periodically so that celebration does not simply become part of routine background noise. Find ways to celebrate that represent the action or event being celebrated.
5. Connect the Dots
Help nurses understand how what they do every day, the actions they take, and the improvements they make help achieve goals. Ideally, every member has helped to create individual and unit goals that roll up to support the organization’s goals, and these staff goals let every person see how they contribute to success.
These individual and unit goals help to promote both personal accountability and teamwork, as people work together to support each other in achieving them. Keeping track of current progress through leading and lagging indicators as well as the aimed-for measure of achievement prominent in the organization’s consciousness, keeps staff focused on where they are and where they are headed.
Ways to connect the dots. Communicate, communicate, communicate through written and verbal messages. Post achievements and progress at the individual, unit, and organizational level in the lounges, break rooms, and on Communication Boards. Help every staff member understand how they have contributed to successes and what they can do to help achieve further success. Make communication of progress a focal point of spoken messages in videos, forums, informal conversations, and formal rounding.
What’s possible when nurses are engaged?
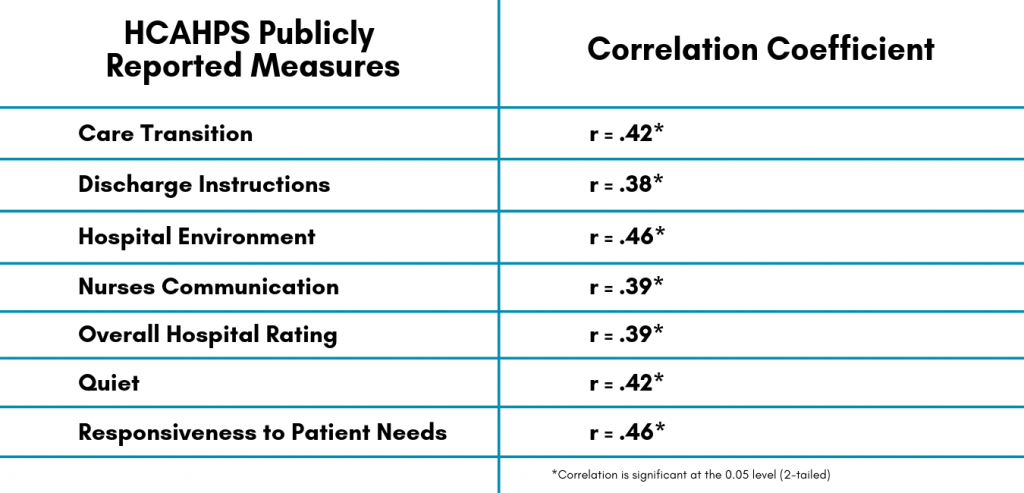
Fully engaged nurses provide organizations with opportunities not previously possible. “Fully engaged nurses are dedicated to the organization, remaining with you through good times and bad, and reducing turnover.”3 In addition, as the PRC Nursing Engagement study demonstrated, patient experience scores improve. These correlations show us that engaged nurses are the people who help to reduce readmissions, improve patients’ experiences of their hospital stays, and increase the quality and safety of care (see Figure 1).3 Finally, this state of engagement allows nurses to be the fully human, highly skilled healthcare providers we want our patients to benefit from in every encounter.
For consultation on improving nurse engagement or reducing nursing turnover, contact Katie Owens, President of the Healthcare Experience Foundation.
References
- Bierhaus, P, Auerbach, D., and Staiger, D. (January-February 2016). Recent changes in the number of nurses graduating from undergraduate and graduate program nursing. ECONOMIC$ Vol. 34, No. 1, p 48.
- Nursing Solutions Inc. 2019 National Health Care Retention and RN Staffing Report.
- King, C. and Bradley, L. (2019). Trends and Implications with Nursing Engagement: PRC National Nursing Engagement Report.
- American Association of Colleges of Nursing (2019). Nursing shortage.
- Owens, K. and Eggers, J. (July 2017). Perspective is everything: evidence to improve engagement. HR Pulse.
- Posted in:
- Compassion & Empathy, Culture, Trust



